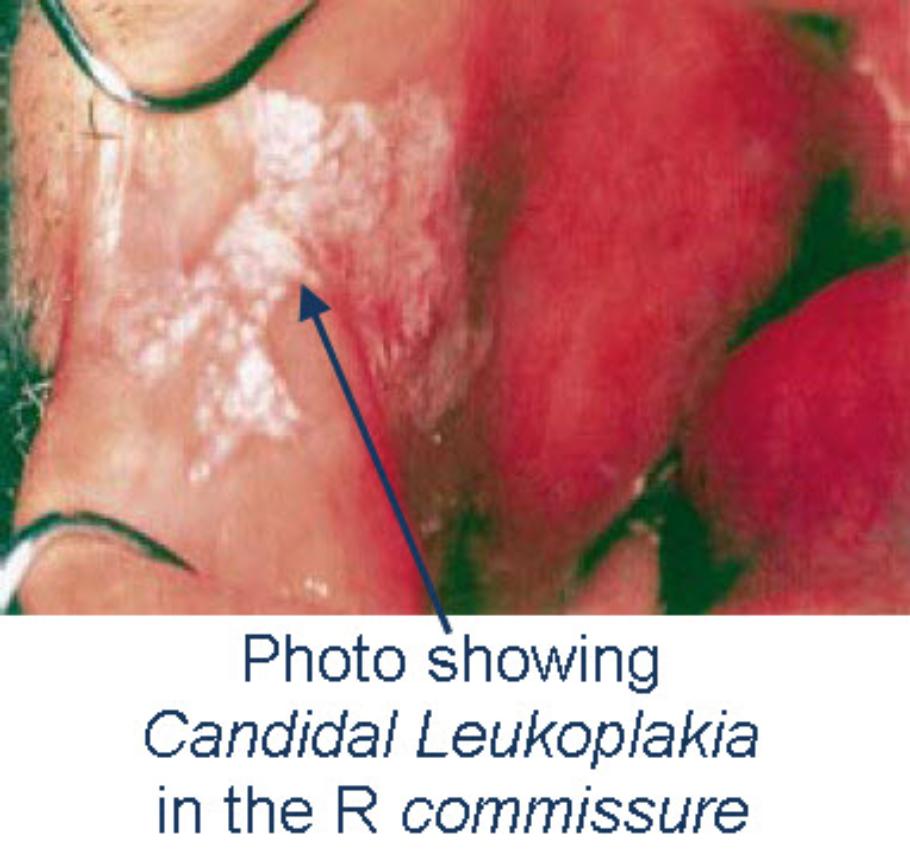
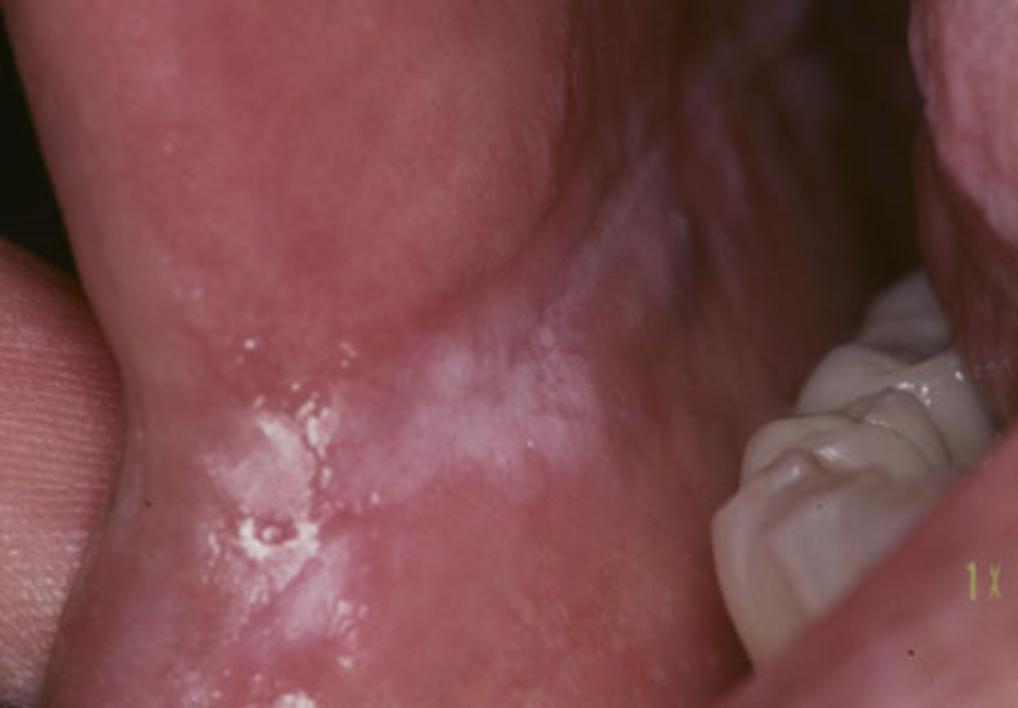
Candidal Leukoplakia
(Chronic Hyperplastic Candidosis / Candidal Epithelial Hyperplasia)
What is Candidal Leukoplakia?
Chronic oral candidosis produces a tough, adherent, white plaque (leukoplakia), distinguishable only by biopsy from other leukoplakias.
Chronic hyperplastic candidiasis or candidal leukoplakia is a persistent white lesion, characterised histologically (under the microscope) by parakeratosis (increased keratin production) and chronic intra epithelial (within skin cells) inflammation with fungal hyphæ (shape of fungus) invading the superficial layers of the epithelium (skin).
Candidal leukoplakia is an uncommon condition found in adults.
The epithelium of some leukoplakias is invaded by Candida hyphæ but it is unclear whether the yeasts are secondary invaders or are causally involved in the development / transformation of leukoplakia.
The cellular changes often include hyperplasia; however, cellular changes can occur that range from mild dysplasia to invasive carcinoma. C. albicans is the species of fungus that is most commonly found in association with candidal leukoplakia. The Candida biotypes associated with candidal mouths.
Candidal leukoplakia may be predisposed to in a minority of patients by:
- smoking
- iron and folate deficiencies
- defective cell-mediated immunity
- blood group secretor status.
What are the signs and symptoms?
Adults, typically males of middle age or over, are affected.
The usual sites are the dorsum of the tongue and the post-commissural buccal mucosa (see photos). The plaque is variable in thickness and rough / irregular in texture or nodular with an erythematous background (‘speckled’). Angular stomatitis may be associated, is sometimes continuous with intra-suggests the candidal nature of the lesion.
Candidal leukoplakias are chronic, discrete, raised lesions that vary from small, palpable, translucent, whitish areas to large, dense, opaque plaques, hard and rough to the touch (plaque-like lesions). Homogeneous areas or speckled areas can be seen, which do not rub off (nodular lesions). Candidal leukoplakias are non-homogeneous ‘speckled’ leukoplakias in up to 50%.
Candidal leukoplakias usually occur on the buccal mucosa on one or both sides, mainly just inside the commissure, less often on the tongue.
How Is It Diagnosed?
Unlike Thrush, the plaque cannot be wiped off but fragments can be detached by firm scraping. Under the microscope, Candidal hyphæ are seen in amongst the epithelial cells. The hyphæ are seen growing (as in Thrush) through the full thickness of the keratin to the prickle cell layer of the skin, where the inflammatory cells tend to be more concentrated.
Electron microscopy shows Candida albicans to be an intra-cellular parasite growing within the epithelial cytoplasm.
Induction of epithelial proliferation by C. albicans infection has been demonstrated experimentally. Dysplasia may be present, especially in speckled lesions.
Candidal leukoplakia should be biopsied both to:
- distinguish it from other non-candidal lesions
- examine for possible dysplasia.
How is it treated?
After confirmation of the diagnosis by histology, treatment should be with a systemic anti-fungal drug such as fluconazole (this may have to be continued for several months). Other factors likely to perpetuate candidal infection should be controlled.
Stopping the patient from smoking and elimination of candidal infection from under an upper denture are important.
Any iron deficiency should also be treated.
Excision of candidal plaque alone is of little value, as the infection can recur in the same site even after skin grafting. Vigorous anti-fungal therapy is therefore essential but sometimes some residual (uninfected) plaque may persist after treatment and lesions often recur and require long-term intermittent anti-fungal therapy.
Prognosis
The potential for malignant change exists. The level of risk is controversial but low (9% to 40% of candidal leukoplakias may develop into carcinomas [cancers]).
Factors influencing the prognosis may include:
risk factors, such as tobacco and alcohol use
whether the lesion is whether the lesion is speckledspeckled (more dangerous) or (more dangerous) or homogeneoushomogeneous
(more dangerous) or (more dangerous) or homogeneoushomogeneous
the presence (more dangerous) and degree of epithelial dysplasia
In order to improve the prognosis:
Tobacco and alcohol habits should be stopped.
Anti-fungals should be used. The lesions of candidal leukoplakia may prove poorly responsive to polyene anti-fungal drugs and, in some cases, respond only to systemic fluconazole.
Excision is indicated if there is more than mild dysplasia.
The patient should be fully informed about the condition and reviewed regularly.