Jaw Joint Problems
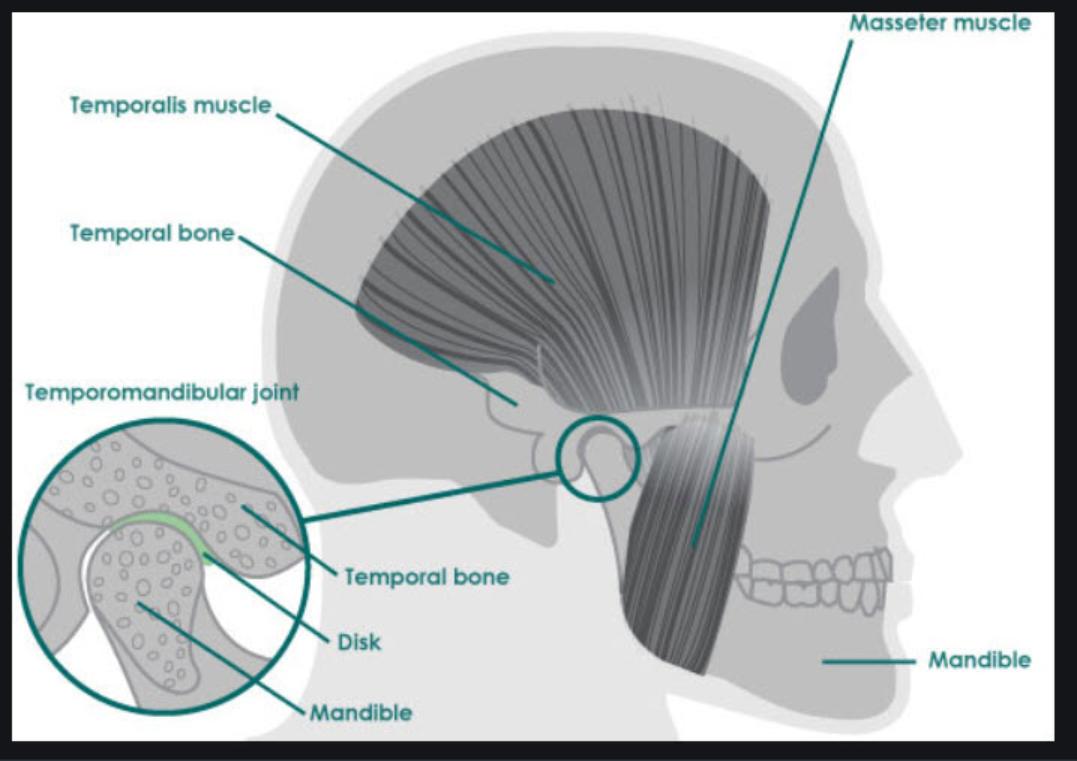
The temporomandibular joint (TMJ / jaw joint) is located in front of the ear where the skull and the lower jaw meet. The joint allows the lower jaw (mandible) to move and function for eating, talking etc. The joint itself is made up of two bones that are separated by a disc of cartilage (a tough tissue). Ligaments and muscles surround the joint.
Problems with the jaw joint are very common but typically only last a few months before getting better. In some instances, only the muscles are affected (known as myofacial pain dysfunction), whereas in others, the cartilage and ligaments may also be a problem (known as internal derangement of temporomandibular joint).
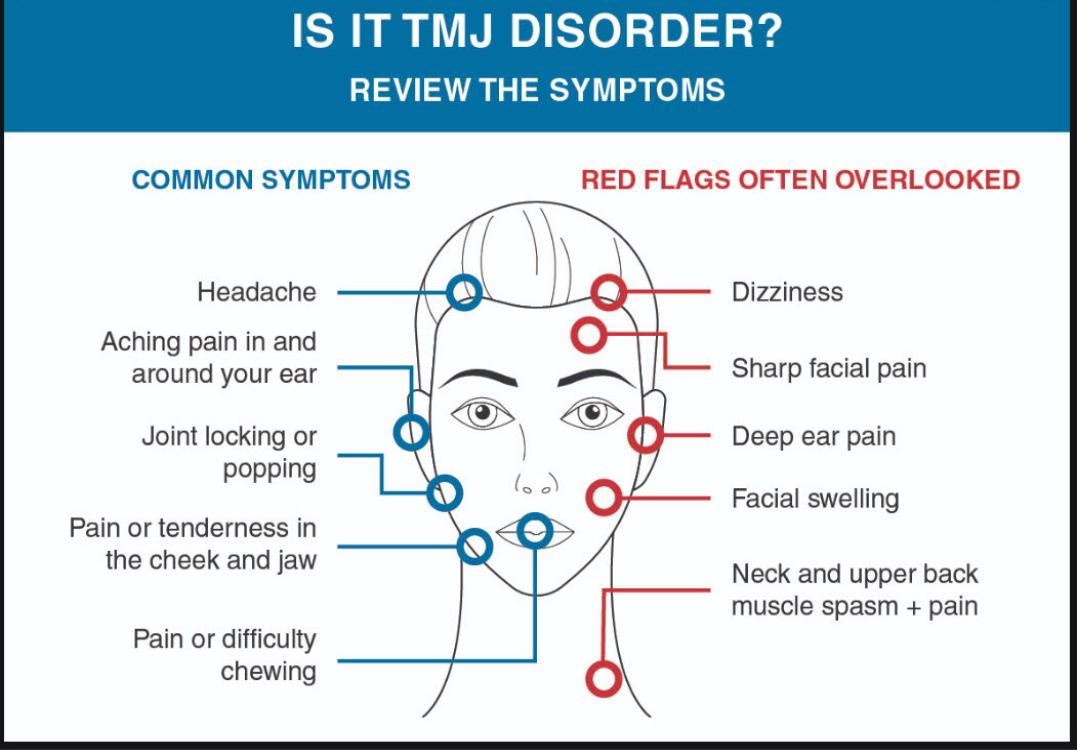
The most common symptoms are:
- Joint noise – such as clicking, cracking, crunching, grating or popping.
- Pain – usually a dull ache in and around the ear. The pain may radiate, i.e. move forwards along the cheekbone or downwards into the neck.
- Headache.
- Trismus – inability to open your mouth fully.
Most jaw joint problems are made worse by chewing and are aggravated at times of stress.
What causes jaw joint problems?
Pain is caused by the muscles in and around the jaw joint tightening up. Joint noise occurs if the disc of cartilage moves out of its normal position between the bones of the jaw joint. Most commonly, the disc slips forward and a noise is made when it returns to its normal position in between the bones. The noise sounds louder to some patients than others because the joint is just in front of the ear. The ligaments and muscles surrounding the joint can in turn go into spasm, producing pain and a difficulty in opening the mouth properly.
The ætiology of jaw joint problems is multi-factorial and includes biological, environmental, social, emotional and cognitive triggers.
Factors consistently associated with jaw joint problems include other pain conditions (e.g., chronic headaches), fibromyalgia, autoimmune disorders, sleep apnœa and psychiatric illness (e.g. depression & anxiety).
Smoking is associated with an increased risk of jaw joint problems in females younger than 30 years.
Classification of Jaw Joint Problems
Jaw joint problems are classified as either as intra-articular (within the joint) or extra-articular (involving the surrounding musculature).
Musculoskeletal conditions are the most common cause of jaw joint problems, accounting for at least 50% of cases.
Articular disk displacement involving the condyle–disk relationship is the most common intra articular cause of jaw joint problems.
Why have I got jaw joint problems?
The cartilage in the jaw joint is thought to slip forwards because of over-use of the muscles surrounding the jaw. The over-use commonly produces tightening of the muscles and may occur as a result of chewing habits, such as grinding or clenching the teeth when under stress (usually when asleep). Nail biting or holding things between the teeth can also cause jaw joint problems. Less commonly, missing back teeth, an uneven bite or an injury to the jaw can lead to the problem. Often, no obvious cause is found.
Are my problems anything to worry about?
Jaw joint problems are usually not serious and do not lead on to other problems, e.g. arthritis of the jaw joint. However, they are a nuisance. Fortunately, jaw joint problems usually respond well to simple treatments.
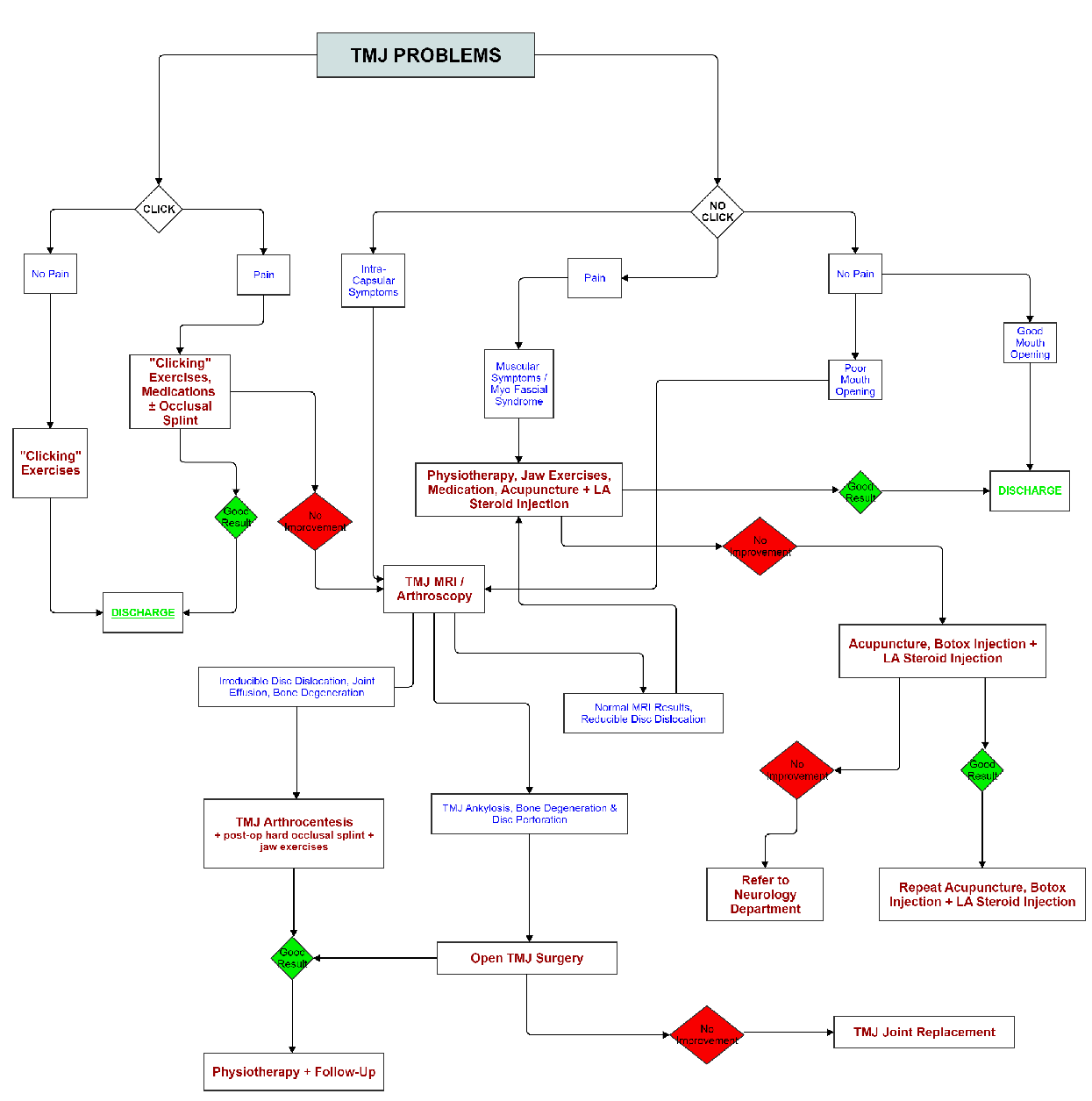
What are the Treatments?
Treatments vary depending on whether you are suffering from myofacial pain dysfunction, internal derangement of the temporomandibular joint or a combination of both. On the whole, treatment is aimed at trying to reduce the workload of the muscles, so allowing the disc of cartilage to return to a normal position in the joint.
This includes such advice as:
- Eat a soft diet that requires little chewing – allowing the over-worked muscles to rest.
- Take painkillers – anti-inflammatory medication (e.g. Ibuprofen) is good and can be taken as either tablets or applied as a gel (such as Ibuprofen gel or Voltarol Gel / Emugel) on the outside of the joint.
- Use heat – e.g. wrap a hot water bottle filled with warm water in a towel and apply it to the side of your face.
- Identify and stop any bad habits, such as clenching or grinding. Although, this may be difficult as they are often ‘subconscious’, i.e. you may not be aware you are doing them.
- Use relaxation therapy and learn techniques to control tension and stress.
- Jaw joint exercises – your doctor will advise you on the best kind of exercises for your problems. Please remember to follow them as instructed.
- Rest the joint as much as possible, e.g. avoid yawning.
- Wear a clear plastic splint that fits over the teeth and is worn mainly at night (a Bite Raising Appliance). This helps support the joint and surrounding muscles.
- Follow a physiotherapy programme.
- Replace missing teeth to balance the bite (if appropriate).
What happens if these methods do not help?
Surgery is only carried out in a small number of cases. This can involve manipulation of the joint whilst you are asleep, or more rarely, surgery carried out with a mini telescope. In extreme cases, it may be necessary to open the joint and operate on the bones, cartilage and ligaments.
Can jaw joint problems develop into anything worse?
It is important to realise that jaw joint problems, although a nuisance, are not sinister and usually respond well to relatively simple measures over a period of time.
Patients can manage most of the treatments themselves.
Occasionally, jaw joint problems may return after several years. It is very rare for jaw joint problems to progress to anything serious, like arthritis.
Useful Articles & Websites
NHS Evidence Clinical Knowledge Summaries
American Academy of Oro-Facial Pain
National Institute of Dental and Craniofacial Research
Dental Health Information Center (Temperomandibular [TMJ] Disorders)
American Society of Temperomandibular Joint Surgeons
American Academy of Otolaryngologists – Head & Neck Surgery
McKinley Health Center, University of Illinois 2002. Temporomandibular Joint Disorders
BAOMS 2003. Jaw Joint Problems
TMJ Disorders (2006) – US Department of Health & Human Services, National Institutes of Health.
BAOS Information Sheet (2006). Temporomandibular (Jaw) Joint Problems
Am Fam Physician 2007. Temporomandibular Joint Disorders
ENT News 2008 – Assessment & Initial Management of TMJ Disorders
J Dent Ed 2008. TMJ Disorders – Future Innovations in Diagnostics & Therapeutics
NEJM 2008. Temporomandibular Disorders
AGRI 2009. Etiology of temporomandibular disorder pain
BJOMS 2009. Leading article. Current Thinking in Temporomandibular Joint Management.
International Dentistry SA 2010. Etiology of temporomandibular disorders – the journey so far
BDJ 2010. Risk management in clinical practice. Part 8. Temporomandibular disorders
British Journal of Pain 2011. Recent Advancements in Temporomandibular Disorders (TMDs)
J Dent 2011. Limited evidence that acupuncture is effective for treating temporomandibular disorders
British J Pain 2011. Recent Advances in Temporomanidular Disorders (TMDs)
Evidence-Based Dentistry 2012. Some Evidence for the Management Temporomandibular Joint Disorders
BDJ 2012. Letter to Editor. TMJ Dysfunction
BJOMS 2012. Oral Presentations. The TMJ MDT clinic — the King’s experience
BDA February 2013 – TMJ – What Should I Do, Who Should I Turn To?
BDJ 2013. Oral Surgery – Part 3. Temporomandibular Disorders
European Pain Federation 2013. Temporomandibular Disorders. Patient Leaflet
Dent Update 2013. Conservative Temporomandibular Disorder Management. What DO I do – FAQ
Eastman Dental Hospital 2013. Temporomandibular Disorder (Primary Care)
Eastman Dental Hospital 2013. Temporomandibular Disorder (Complex)
Int J OMF 2013. A New Surgical Classification for TMJ Disorders
US Dept Health & Human Services, Nat Institute of Health 2013. TMJ Disorders
American Academy of Orofacial Pain 2014. Temporo-Mandibular Joint Disorders
BJOMS 2014. Temporomandibular joint multidisciplinary team clinic
Am Fam Physician 2015. Diagnosis & Treatment of Temporomandibular Disorders
BMJ 2015. Clinical Review. Temporomandibular Disorders
Dental Press J Orthod. 2015. TMD & Chronic Pain – A Current View
Dent Update 2016. Pain Part 6. Temporomandibular Disorders
Austral Dent J 2018. Management of Temporomandibular Joint Disorders – A Surgeon’s Perspective
Intech 2018. Nonsurgical Strategies for the Treatment of Temporomandibular Joint Disorders