Oral Cancer – Ætiological Factors
More than 90% of Oral Cancer is Oral Squamous Cell Carcinoma (OSCC).
OSCC accounts for approx 2 – 4% of all cancers in the UK but is one of the most common cancers on the Indian subcontinent.
Men are more frequently affected than women; most OSCC patients > 40 and the incidence of rises rapidly with age.
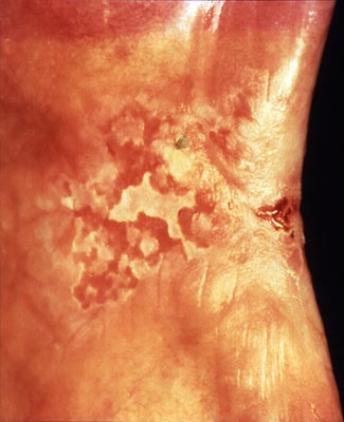
The lower lip is the most common site & related to actinic (sun / solar) damage.
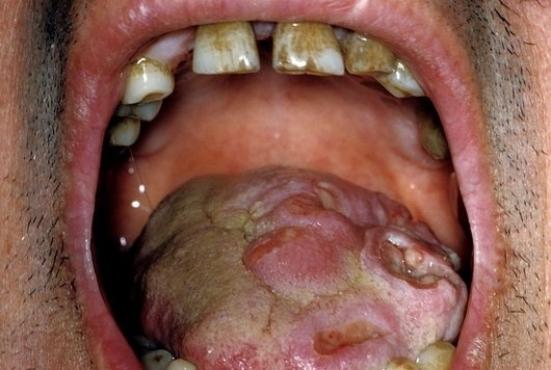
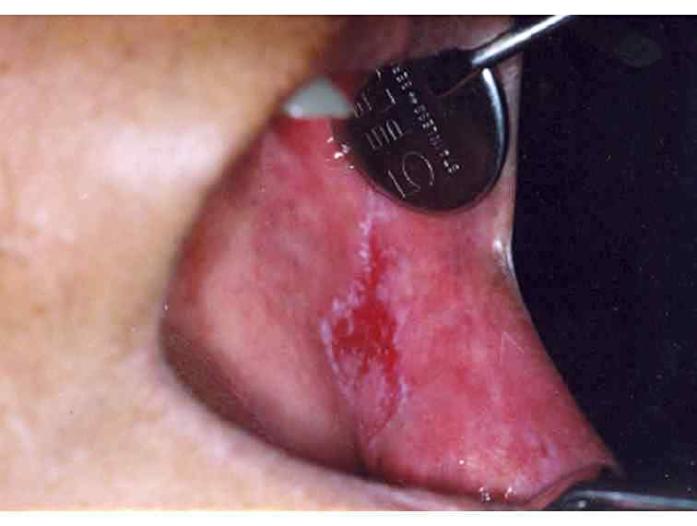
The tongue (the sides especially further back [postero-laterally]), is the most common site within the mouth.
Heavy tobacco smoking & alcohol consumption tend to be associated with the development of OSCC; in India & SE Asia, betel & areca nut chewing may be more important.
Ætiological Factors for Oral Cancer
Carcinogens
- Tobacco
- Alcohol
- Areca nut / betel
Sunlight (lip only)
Infections
- Syphilis (Syphilitic leukoplakia)
- Candidiasis (Candidal leukoplakia)
- Viruses (HPV)
Mucosal Diseases
- Dysplastic lesions
- Oral Lichen Plamus
- Oral Sub-Mucous Fibrosis
Genetic Disorders
- Dyskeratosis congenita
- Fanconi’s anæmia
Syphilis (Syphilitic Leukoplakia / Glossitis)
Syphilitic leukoplakia, especially of the tongue dorsum is a feature of tertiary syphilis (rarely seen now) but the malignant potential is high.
Carcinoma developing near the centre of the tongue dorsum is typically the sequel to syphilitic leukoplakia. Given the decline in late-stage syphilis, it is exceedingly rare in this site now.
Human Papilloma Virus 16 (HPV 16)
HPV related cancers appear to occur on the tonsillar area, the base of the tongue and the oro-pharynx (non-HPV positive tumours tend to involve the anterior tongue, floor of the mouth, the mucosa that covers the inside of the cheeks and alveolar ridges).
In general, it appears that HPV-positive tumours occur most frequently in a younger group of individuals than tobacco-related malignancies. They occur more in white males and in non-smokers. The HPV-positive group is the fastest growing segment of the oral cancer population.
It does not appear that the HPV 16 acts synergistically with tobacco or alcohol and represents a completely unique disease process.
Oral Lichen Planus
It is estimated that 1 – 4% of patients develop carcinomata after a decade. Plaque-like & erosive OLP in unusual sites (such as the fauces & tongue) should be regarded with suspicion.
In view of the commonplaceness of OLP, its importance as a pre-malignant lesion may be considerable.
Cutaneous LP appears to carry no risk of malignant change.
SMF affects those from the Indian sub-continent & SE sclerosis but limited to the oral tissues & without the immune abnormalities.
Arecoline, a stimulant derive from the areca nut is thought to induce fibroblast proliferation & collagen synthesis.
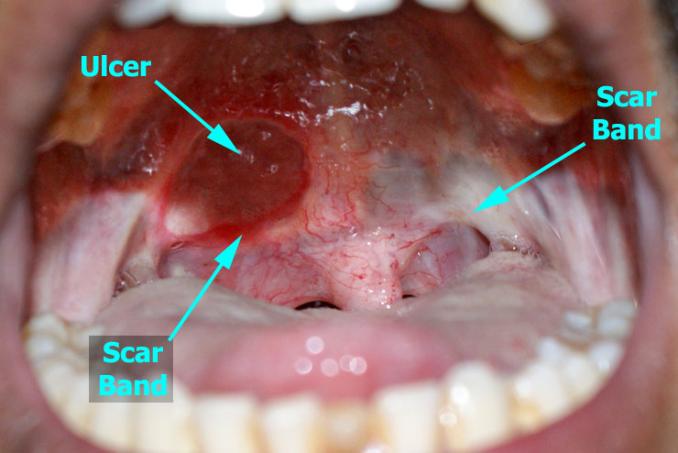
Clinically, there is symmetrical fibrosis (scarring) of the buccal mucosæ, soft palate & the inner aspects of lips.
The overlying mucosa may be normal or there may be a vesiculating stomatitis. Fibrosis & ishæmia causes extreme pallor of the affected area which becomes so hard that it can’t be indented by your finger.
Progressive trismus making it very difficult to eat / drink. Malignant change is from 4.5 – 8 %.
Useful Articles & Websites
Dental Protection. Risk Management Module. Oral Cancer.
Preventive Dentistry 2006. Oral Cancer – A Growing Concern.
Oral Oncology 2009. Review. Global epidemiology of oral and oro-pharyngeal cancer.
BMJ 2010. Head & Neck cancer – Part 1. Epidemiology, presentation & prevention.
JADA 2011. Rise in Oral Cancer Linked to HPV, Study Shows
BDJ 2013. HPV linked to a third of throat cancer cases
BDJ 2013. Letters to the Editor. Tongue Cancer Subgroup
Dent Update 2015. Mouth Cancer for Clinicians Part 3. Risk Factors (Traditional – Tobacco)
Dent Update 2015. Mouth Cancer for Clinicians Part 5. Risk Factors (Other)
BDJ 2018. Oral Cancer & Tobacco – Developments in Harm Reduction
BDJ 2018. The Changing Epidemiology of Oral Cancer – Definitions, Trends & Risk Factors
Dental Update 2020. Mouth Cancer − Risk Factors & Potentially Malignant Disorders