Cervico-Fascial Infections & Ludwig’s Angina
Cervico-Fascial Space Infections / Cervico-Facial Cellulitis / Peri-Mandibular Infections
Due to the strategic position of the wisdom tooth (3rd molar) at the junction of a number of different fascial spaces, any infection in this area must be taken seriously as an infection here can easily spread along the fascial planes and compromise the airway.
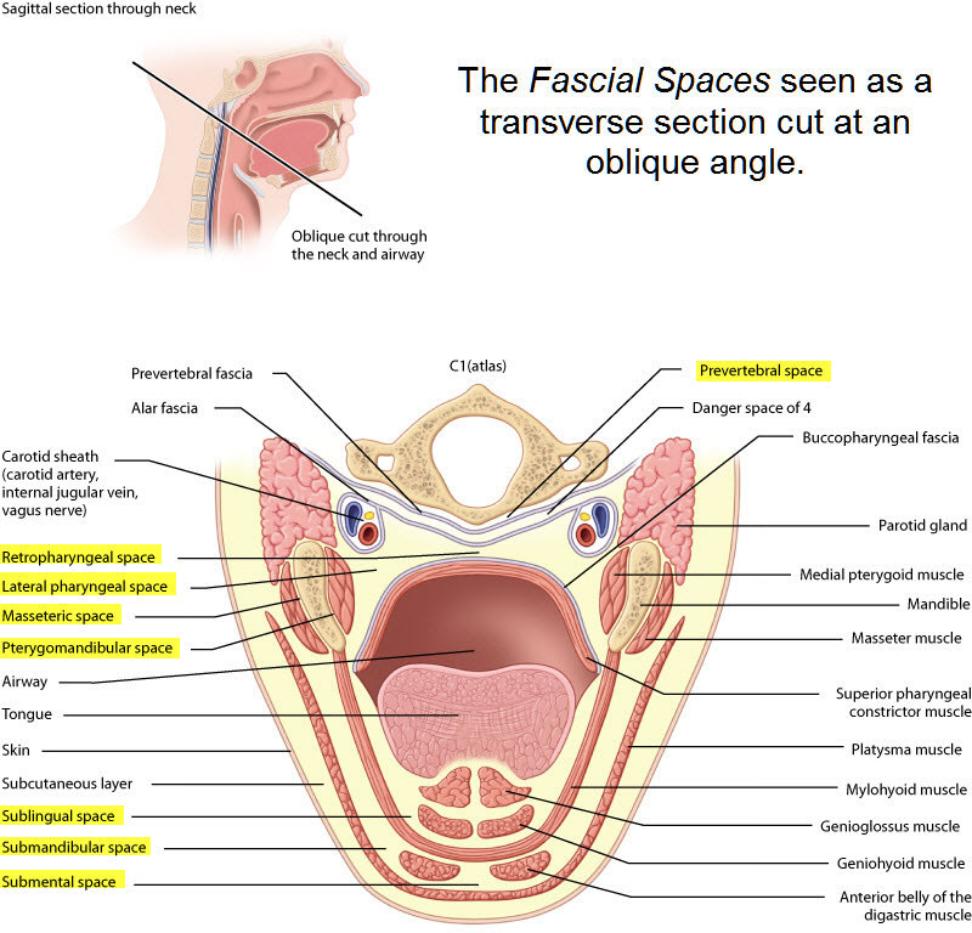
The head and neck (cervical) region has a large number of fascial spaces. These ‘spaces’ are bounded by the fascia, which may stretch or be perforated by the purulent exudates (pus), facilitating the spread of infection. These ‘spaces’ are potential areas and do not exist in healthy individuals. There are a number of them including the:
- buccal space
- buccinator space
- para-pharyngeal space
- sub-mandibular space
- sub-lingual space
- lateral pharyngeal and
- pterygoid space
Infections in the buccal space and buccinator space are usually localised on the lateral side of the mandible.
Sub-masseteric infections occupy the potential space between the lateral border of the mandible and the masseter muscle. This is not a fascial-lined space; infection in this area is in direct contact with the masseter muscle and usually induces intense spasm in the muscle, resulting in a profound limitation in mouth opening (trismus).
Internal pterygoid space infections occupy the fascia-lined space between the internal pterygoid muscle and the medial aspect of the mandible. Infections in this area cause a less profound trismus but can result in airway embarrassment. They can also result from Inferior Alveolar Nerve block.
The sub-mandibular space consists of a splitting of the investing fascia of the neck to enclose the submandibular salivary gland and is in continuity with the internal pterygoid and para-pharyngeal spaces. Infections in this region can cause airway embarrassment and, when bilateral with associated cellulitis, is termed Ludwigs Angina. This is very serious and potentially life-threatening.
Infections occur between the pharyngeal mucosa and superior constrictor muscle. Infections in this region are also potentially life-threatening and require urgent attention.
Fascial Space Infections – key features
- Potentially life-threatening infections due to spread of bacteria into peri-oral fascial spaces
- Infection usually arises from lower second or third molars (wisdom teeth).
- Affected tissues are swollen and of ‘board-like’ hardness
- Severe systemic upset
- Glottic œdema (swelling) or spread into the mediastinum may be fatal
The main principles of treatment remain surgical with (dependent) drainage of pus augmented by antibiotic therapy. The infective organisms are normal oral flora and the penicillin family of antibiotics remains the antibiotics of first choice.
With the increasing recognition of the role of anærobic oral bacteria in these infections, clindamycin can be substituted for penicillin in severe infections or metronidazole added to the penicillin. Studies show an average of four bacterial species in any oral infection with anærobic species outnumbering ærobic species, although streptococci remain the largest single group of organisms.
Ludwig’s Angina
Ludwig’s Angina is a severe form of cervico-fascial infection / cellulitis which usually arises from the lower second or third molars (wisdom teeth).
Deep fascial space infections cause gross inflammatory exudates (a fluid with a high content of protein and cellular debris which has escaped from blood vessels and has been deposited in tissues or on tissue surfaces, usually as a result of inflammation. It may be septic or non-septic) and tissue œdema (swelling), associated with fever and toxæmia (blood poisoning). Before the advent of antibiotics, the mortality was high and the disease is still life-threatening if treatment is delayed.
The main fascial spaces involved in Ludwig’s Angina are the sublingual, submandibular and para-pharyngeal. Normally, the spaces both side of the midline (ie bilateral) are effected.
The characteristic features are:
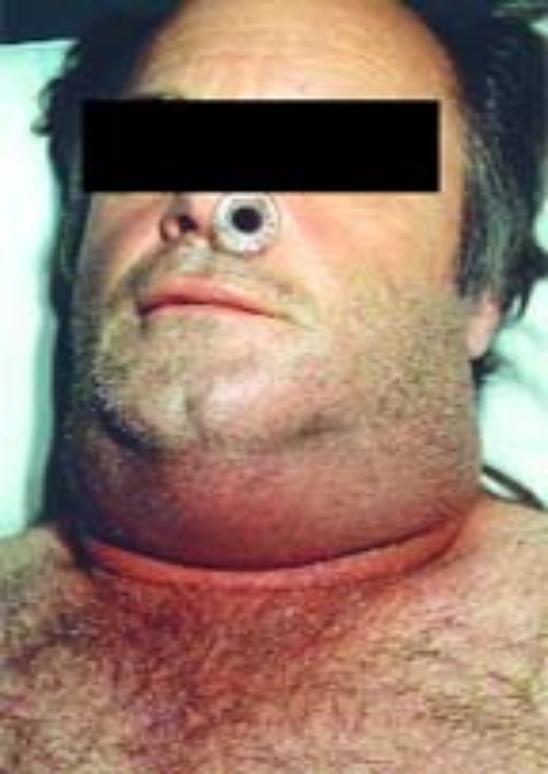
- diffuse swelling, pain, fever and malaise.
- The swelling is tense and tender, with a characteristic ‘board-like’ firmness.
- The overlying skin is taut and shiny.
- Pain and œdema (swelling) that limit opening the mouth and often cause dysphagia (difficulties in swallowing)
- Systemic upset is severe, with worsening fever, toxæmia (blood poisoning) and leucocytosis.
- The regional lymph nodes are swollen and tender.
- In Ludwig’s Angina particularly, airway obstruction can quickly result in asphyxia.
Pathology
Anærobic bacteria are primarily responsible and infection mainly spreads from mandibular third molars (lower jaw wisdom teeth) whose apices (root tips) are closely related to several fascial spaces. Fasciæ, covering muscles and other structures are normally adherent but can be spread apart by inflammatory exudate.
Spaces created in this way are almost avascular (do not have a blood supply) and inflammatory exudate carries bacteria widely through them. It involves the sub-lingual and sub-mandibular spaces bilaterally (on both sides) almost simultaneously; it readily spreads into the lateral pharyngeal and pterygoid spaces and can extend into the mediastinum. The main features are rapidly spreading sub-lingual and sub-maxillary cellulitis with painful, brawny swelling of the upper part of the neck and the floor of the mouth on both sides. With involvement of the para-pharyngeal space, the swelling tracks down the neck and œdema can quickly spread to the glottis.
Swallowing and opening the mouth become difficult and the tongue may be pushed up against the soft palate. The latter or œdema of the glottis causes worsening respiratory obstruction. The patient soon becomes desperately ill, with fever, respiratory distress, headache and malaise.
Management
The main requirements are:
- immediate admission to hospital
- procurement of a sample for culture and sensitivity testing
- aggressive antibiotic treatment
- securement of the airway by tracheostomy if necessary, and
- drainage of the swelling to reduce pressure.
Useful Articles & Websites
J Can Dent Assoc 2001. A Rare Complication of Tooth Abscess – Ludwig’s Angina & Mediastinitis
BDJ 2007. Death from Overwhelming Odontogenic Sepsis – A Case Report
Cases J 2008. Ludwig’s Angina & Airway Considerations – A Case Report
Int J Emerg Med 2010. Clinical Images. Ludwig’s Angina
Int J Otorhinolaryngol 2011. Ludwig’s Angina – A Controversial Surgical Emergency. How We Do It
J Pharm Sci & Res 2014. Ludwig’s Angina – Causes, Symptoms & Treatment
BMJ 2015. Management of Severe Acute Dental Infections
J Health Sci Res 2017. Ludwig’s Angina – Emergency Treatment
BDJ 2018. Management of Odontogenic Infection at a District General Hospital