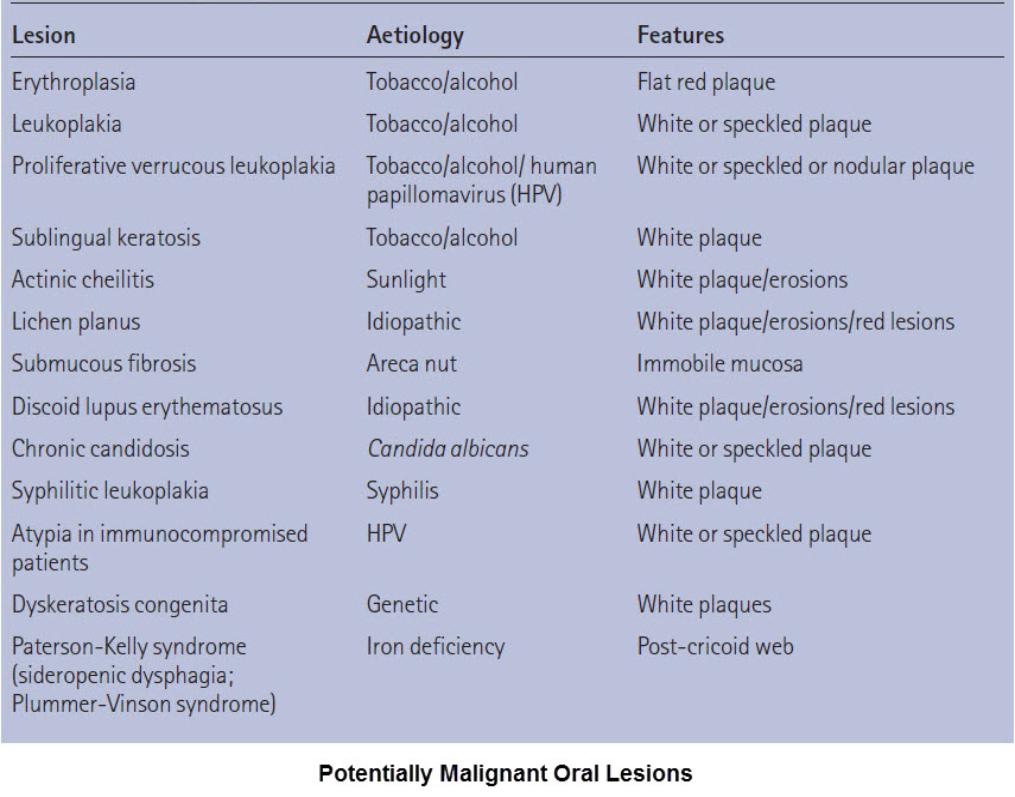
Oral Cancer – Pre-Malignant Lesions
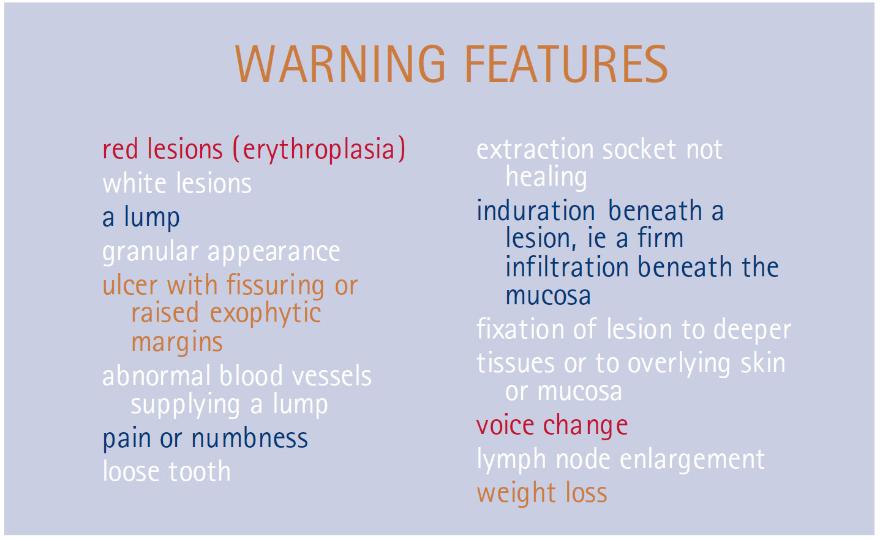
Most oral cancers appear to arise in ‘normal’ oral mucosa but some are preceded by potentially malignant / pre-malignant clinically obvious lesions.
These include:
- Actinic Cheilitis
- Erythroplakia / Erythroplasia (Red Patch)
- Leukoplakia (White Patch)
- Speckled Leukoplakia
- Verrucous Leukoplakia
Conditions that MAY predispose to malignancy (ie oral cancer) include:
- Lichenoid lesions + Lichenoid Dysplasia
- Sub-Mucous Fibrosis
- Previous oral malignancy
- Syphilitic Leukoplakia / Glossitis
- Immunosupression
- Dyskeratosis Congenita
- Paterson-Kelly syndrome
- Discoid Lupus Erythematosis
What are thought to be the lesions / conditions likely to cause malignancy are logically the same ones that cause pre-malignancy.
Actinic Cheilitis (AKA Actinic Keratosis of Lip, Solar Keratosis, Solar Cheilosis)
- Occurs in adults & mainly men
- Mainly seen in persons from the Tropics
- Chronic pre-malignant keratosis of the lip caused by long exposure to solar irradiation. Most is seen:
- on the lower lip with sparing of the commissures
- in fair-skinned men
- 4 – 8th decade of life
- outdoor jobs / activities
- Early stages – erythema & œdema; later stages, the lip becomes dry, scaly & wrinkled with grey / white changes in pigmentation. Lesions appear as a smooth or scaly, friable patch or even the whole lip. Later still, the lip becomes thickened with small greyish-white plaques with even warty nodules forming
- Prevention with sunblocks
- Treatment with topical chemo-exfoliants & surgery
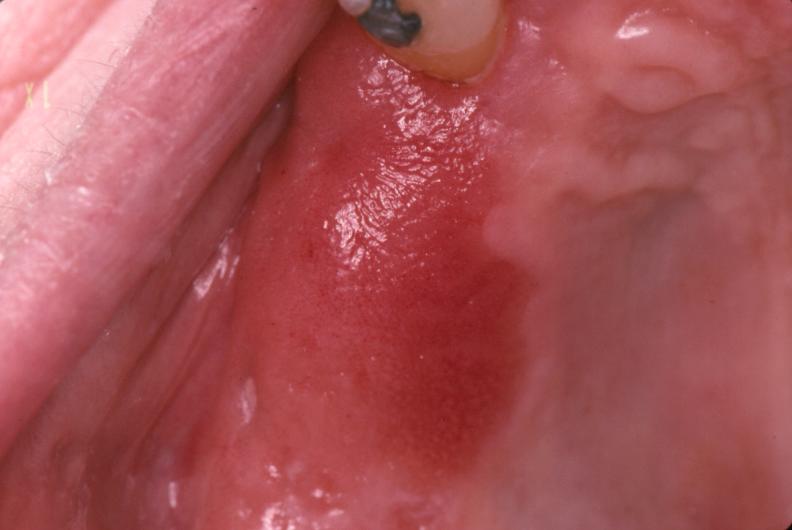
Erythroplasia / Erythroplakia (AKA Red Patch)
- Occurs in the middle aged & the elderly & mainly in men
- Less common than leukoplakia
- Erythroplakia contains areas of dysplasia, carcinoma in situ or invasive carcinoma in virtually every case
Most potentially malignant of all oral mucosal lesions.
- Red velvety patch of variable configuration, usually level / depressed with surrounding mucosa, commonly on the soft palate, floor of mouth or the buccal mucosæ
- Some erythroplakias are associated with white patches & hence termed, speckled leukoplakias
- Any causal factor, such as tobacco, should be stopped
- Lesions removed followed by regular follow-ups
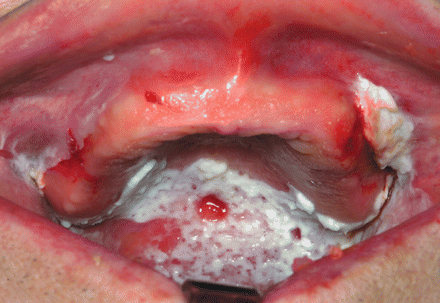
Leukoplakia (AKA White Patch)
- Occurs in approx 1% of the population; men > women
- Predisposing habits – tobacco, alcohol & betel use; sanguinarine use
- Leukoplakia has a wide range of clinical presentations, from homogenous white plaques (faintly white – very thick & opaque) to nodular white lesions to lesions admixed with red lesions.
The malignant potential depends on appearance, site & some ætiological factors.
- Appearance – non-homogenous / heterogenous leukoplakias has a high risk of malignant transformation
- Site – soft palate complex, ventro-lateral tongue & FOM have a high risk of malignant transformation
- Ætiology – virus (HPV, EBV), bacterial (syphilis) or fungal (Candida) have a high risk of malignant transformation
- Any causal factor, such as tobacco, should be stopped.
- Lesions removed followed by regular follow-ups.
- Surgical / Medical treatment
Dysplasia seems to be the most predictive marker in use for malignant potential.
Factors Predictive of Future Malignant Transformation may include:
- History of cancer of upper aero-digestive tract
- Expression of P53 tumour suppressor protein
- Changes involving chromosomes 3p or 9p; “Loss of Heterozygosity” LOH
- Chromosomal polysomy
Principles of Management of Dysplastic Lesions:
- Stop any associated habits, eg betel quid or smoking
- Treat any candidal infection and / or iron deficiency if present
- Biopsy to assess dysplasia
- Assess risk of pre-malignant change on clinical & histological findings
- Consider ablation of individual lesions
- Maintain observation for signs of malignant change
Options for the Management of Pre-Malignant Lesions:
- Observation for early detection of cancer
- Surgical excision with grafting (if required)
- Cryotherapy
- Laser excision / vaporisation
- Topical chemotherapy (eg bleomycin)
- Retinoids
Cryotherapy heals rapidly to leave an apparently normal mucosa. However, there is some uncertainty about the risk of OSCC subsequently arising in these sites.
With laser ablation, seemingly similar concerns.
Topical chemotherapy are largely ineffective and lesions that resolve, recur on cessation of the drugs.
Useful Articles & Websites
Dental Update 1999. Update on Precancerous Lesions
CA Cancer J Clin 2002. Oral Cancer and Precancerous Lesions
BDJ 2003. Oral Cancer Prevention & Detection in Primary Healthcare
Preventive Dentistry 2006. Oral Cancer – A Growing Concern
Dental Update 2006. Current Concepts in the Management of Oral Cancer
Oral Oncology 2009. Review. Global Epidemiology of Oral and Oro-Pharyngeal Cancer
Head Neck 2009. Treatment & Follow-up of Oral Dysplasia – A Systematic Review & Meta-Analysis
BJOMS 2011. Management of Oral Carcinoma – Benefits of Early Pre-Cancerous Intervention
Dent Update 2015. Mouth Cancer for Clinicians Part 5. Risk Factors (Other)
Dent Update 2015. Mouth Cancer for Clinicians Part 6. Potentially Malignant Disorders
British Dental Journal 2018. Oral Cancer & Tobacco – Developments in Harm Reduction