Bruxism / Tooth Grinding
Bruxism (from the Greek βρυγμός “gnashing of teeth”) is characterized by the grinding of the teeth and is typically accompanied by the clenching of the jaw.
It is an oral para-functional activity that occurs in most humans at some time in their lives.
In most people, bruxism is mild enough not to be a health problem. While bruxism may be a diurnal (during the day) or nocturnal (during the night) activity, it is bruxism during sleep that causes the majority of health issues and can even occur during short naps.
Bruxism is one of the most common sleep disorders.
Causes
Bruxism is more accurately classified as a habit.
Some bruxism activity is rhythmic (like chewing) though some activity is sustained (clenching). Researchers classify bruxism as “a habitual behaviour and a sleep disorder”.
Most bruxists are not aware of their bruxism and only 5% go on to develop symptoms, such as jaw pain and headaches, which will require treatment. In many cases, a sleeping partner / parent will notice the bruxism before the person experiencing the problem becomes aware of it.
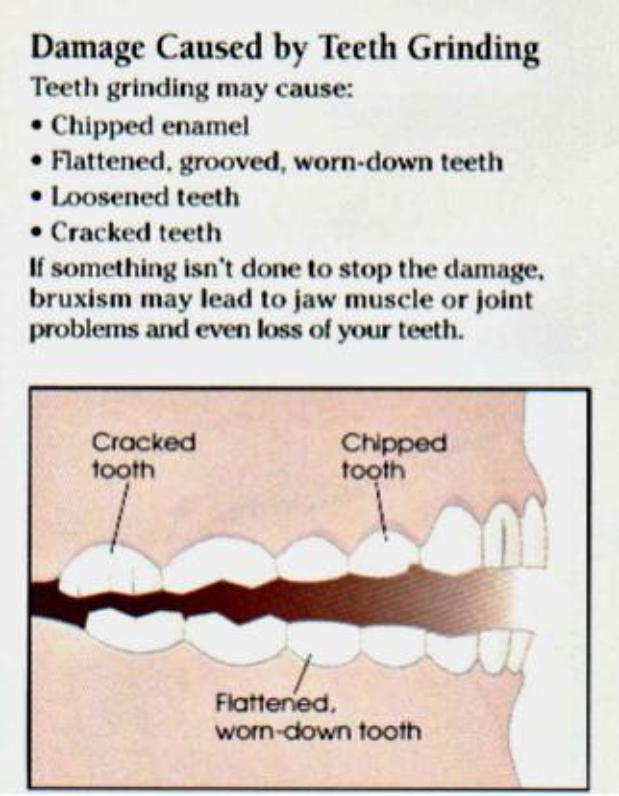
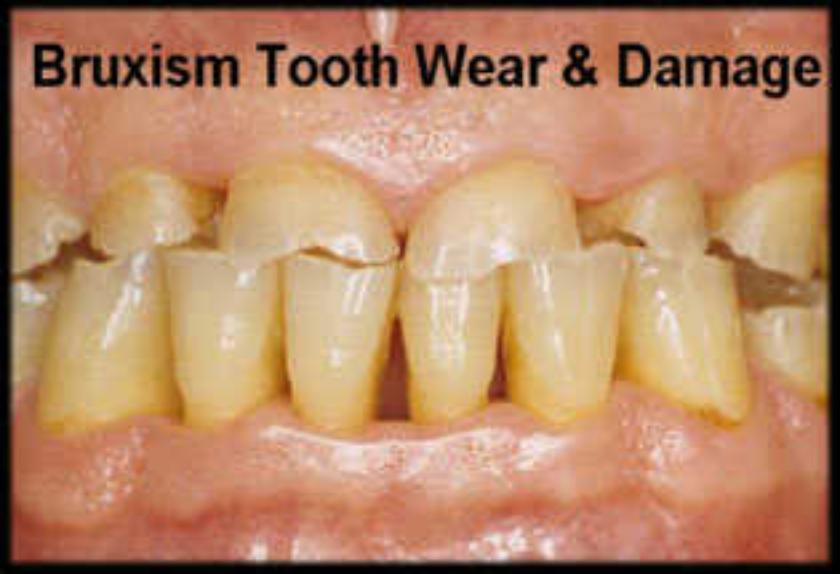
Bruxism can result in abnormal wear patterns of the biting surfaces of the teeth, abfractions and fractures in the teeth. This type of damage is categorised as a sign of occlusal trauma.
Over time, dental damage will usually occur. Bruxism is the leading cause of occlusal trauma and a significant cause of tooth loss and gum recession.
In a typical case, the canines and incisors of the opposing jaws are moved against each other laterally, i.e. with a side-to-side action, by the chewing muscles that lie on the inside of the jaw joints (medial pterygoid muscles). This movement abrades tooth structure and can lead to the wearing down of the biting (incisal) edges of the teeth. People with bruxism may also grind their back (posterior) teeth, which will wear down the cusps of the biting surface of the teeth.
Bruxism can be loud enough to wake a sleeping partner. Some individuals will clench the jaw without significant lateral movements. Teeth hollowed by previous decay (caries) or dental drilling, may collapse, as the cyclic pressure exerted by bruxism is extremely taxing on the tooth structure.
Symptoms
Patients may present with a variety of symptoms, including:
- Anxiety, stress and tension
- Depression
- Earache
- Eating disorders
- Headache
- Insomnia
- Sore / painful jaw
Associated Factors
The following factors are associated with bruxism:
- High levels of anxiety, stress, work-related stress, irregular work shifts, stressful profession and ineffective coping strategies
- Relatively high levels of consumption of caffeinated drinks and foods, such as coffee, colas, and chocolate
- High levels of blood alcohol
- Smoking
- Disturbed sleep patterns and other sleep disorders (obstructive sleep apnea, hypopnea, snoring, moderate daytime sleepiness)
- Malocclusion, in which the upper and lower teeth occlude in a disharmonic way, e.g., through premature contact of back teeth
- Drug use, such as the newer antidepressants (SSRI’s) and stimulants (such as ecstasy, MDA and amphetamines)
- Hypersensitivity of the dopamine receptors in the brain
- GHB and similar drugs when taken with high frequency
- Disorders such as Huntington’s and Parkinson’s diseases
- Obsessive Compulsive Disorder
Treatment
Bruxism may be reduced or even eliminated when the associated factors, e.g., sleep disorders, are treated
successfully.
Although there is no single accepted cure for bruxism, there are a number of treatments available.
- Mouthguards & Splints
- Habit Breakers
- Nociceptive Trigeminal Inhibitor
- Biofeedback
- Cognitive Behavioural Therapy
- Botox
- Dietary Supplements
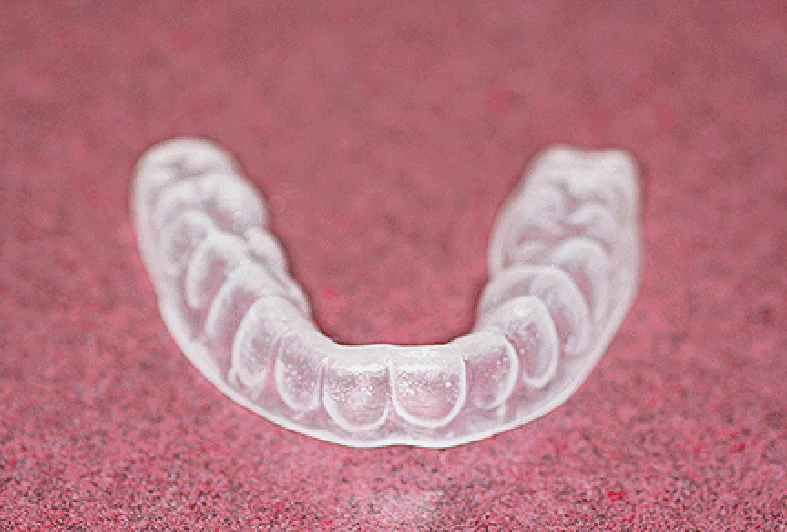
Mouthguards & Splints
Ongoing management of bruxism is based on minimising the abrasion of tooth surfaces by the wearing of an acrylic / soft plastic dental guard or splint (Bite Raising Appliances, BRA’s), designed to the shape of an individual’s upper or lower teeth. These are made by dentists.
BRA’s are thought to work in the following ways:
- constraining bruxism so that damage to the TMJ joints is prevented
- stabilisation of the occlusion by minimising the gradual changes to the positions of the teeth that typically occur with bruxism
- prevention of tooth damage and
- assist a dentist to judge – in broad terms – the extent and patterns of bruxism through examination of the physical indentations on the surface of the splint.
A BRA is typically worn on a long-term basis every night.
Although BRA’s are a first response to bruxism, they do not in fact help cure it. Professional treatment is recommended to ensure proper fit, make ongoing adjustments as needed and check that the occlusion (bite) has remained stable. Monitoring of the BRA is suggested at each dental visit.
Another type of device sometimes given to a bruxist is a repositioning splint.
A repositioning splint may look similar to a traditional BRA but is designed to change the bite (occlusion) of the patient. Scientific studies of these devices generally showed no benefit over more conservative therapies.
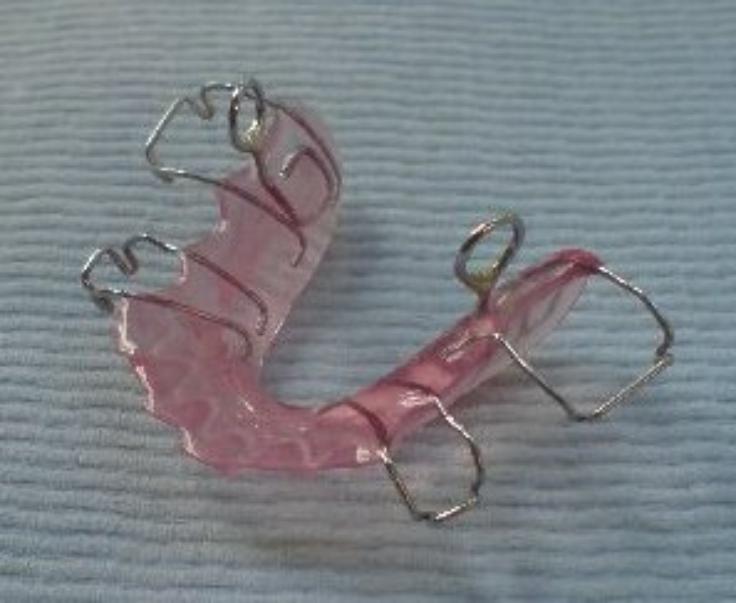
Habit Breakers
This is a development of a BRA’s. These are worn mainly at night. When the patient clenches, the metal ‘projections’ impinge on the roof of the mouth. This would wake or disturb the sleep of the clencher and would theorectically break the habit (eventually).
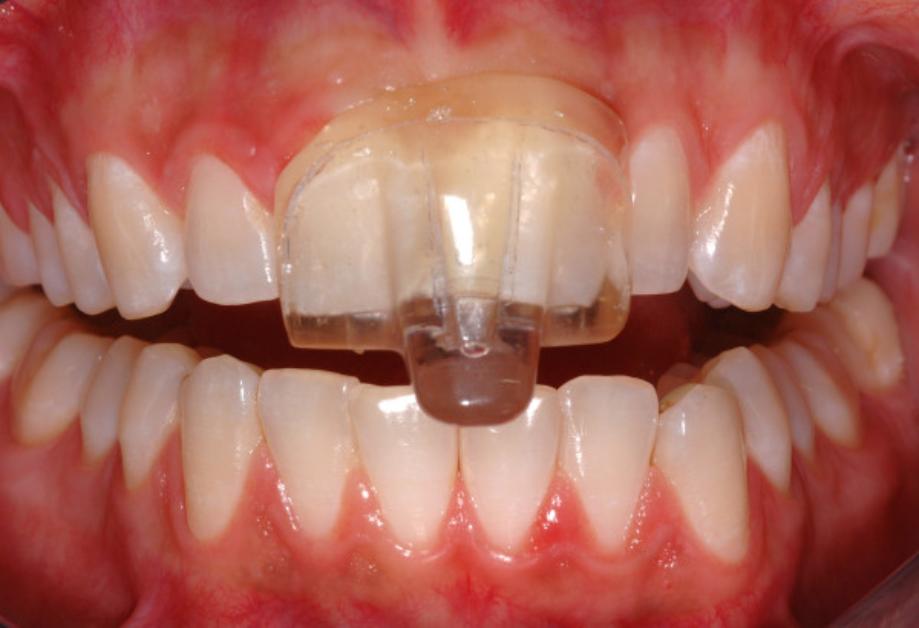
Nociceptive Trigeminal Inhibitor Device / Appliance
The NTI appliance fits on top of the teeth and alters the angle at which the jaw opens, by covering only the front teeth and preventing the molars from coming into contact with each other, thus limiting the contraction of the temporalis muscle. When the grinding starts in the night, the pressure which is applied to the incisors can, it is claimed, send an alarm signal to the brain.
The NTI device must be fitted by a dentist.
The efficacy of such devices is debated. Some writers propose that irreversible complications can result from the long-term use of mouthguards and repositioning splints.
Bio-Feedback
Various bio-feedback devices are currently available and effectiveness varies significantly depending on whether the bio-feedback is used only during waking hours or during sleep as well.
Many authorities remain unconvinced of the efficacy of ‘daytime-only’ bio-feedback.
The efficacy of bio-feedback delivered during sleep can depend strongly on daytime training, which is used to establish a Pavlovian response to the bio-feedback signal that persists during sleep.
Cognitive Behavioural Therapy
Cognitive Behavioural Therapy (CBT) aims to help the patient to manage their problems by changing how they think and act.
CBT encourages the patient to talk about:
- how they think about themselves, the world and other people
- how what the patient does affects their thoughts and feelings
By talking about these things, CBT can help the patient to change how the patient thinks (‘cognitive’) and what the patient does (‘behaviour’), which can help the patient feel better about life.
Botox
Botulinum toxin (Botox) can be successful in lessening effects of bruxism.
Bruxism can also be regarded as a disorder of repetitive, unconscious contraction of the masseter muscle (the large muscle that moves the jaw). In the treatment of bruxism, Botox works to weaken the muscle enough to reduce the effects of grinding and clenching but not so much as to prevent proper use of the muscle. Injections must be repeated more than once per year.
The symptoms that can be helped by this procedure include:
- Grinding and clenching
- Morning jaw soreness
- TMJ pain
- Muscle tension throughout the day
- Migraines triggered by clenching
- Neck pain and stiffness triggered by clenching
The effects last for about three months. The muscles wither (atrophy), however, so after a few rounds of treatment, it is usually possible either to decrease the dose or increase the interval between treatments.
Other authorities caution that Botox should only be used for temporary relief for severe cases and should be followed by diagnosis and treatment to prevent future bruxism or jaw clenching, suggesting that prolonged use of Botox can lead to permanent damage to the jaw muscle.
Dietary Supplements
There is anecdotal evidence that suggests taking certain combinations of dietary supplements may alleviate bruxism; pantothenic acid, magnesium and calcium are mentioned on dietary supplement websites.
Calcium is known to be a treatment for gastric problems, and gastric problems such as acid reflux are known to increase bruxism. Placing whole cloves at night inside the mouth is suggested to have an effect on the jaw’s muscle by relaxing it, yet evidence of this remains largely anecdotal without future research.
Useful Articles & Websites
Dental Update 2018. Occlusal Splints for Bruxing and TMD – A Balanced Approach
Nociceptive Trigeminal Inhibition-Tension Suppresion System
Nociceptive Trigeminal Inhibition Tension Suppression System – How Does It Work
Royal College of Psychiatrists
The Daily Mail, March 2009 – How to stop teeth-grinding … with a little help from Botox
American Dental Association 2005. Do You Grind Your Teeth?
Vital Summer 2011. Raising awareness of bruxism
American Academy of Oral Medicine 2008. Patient Information Sheet. Tooth Clenching or Grinding
Bruxism (Teeth Clenching or Grinding) Advice, Links, Resources
BBC News – Why are we grinding our teeth so much?
BBC Case Notes – The Jaw (also covers bruxism)
The Times, March 2009 – Q&A: How to deal with grinding teeth.