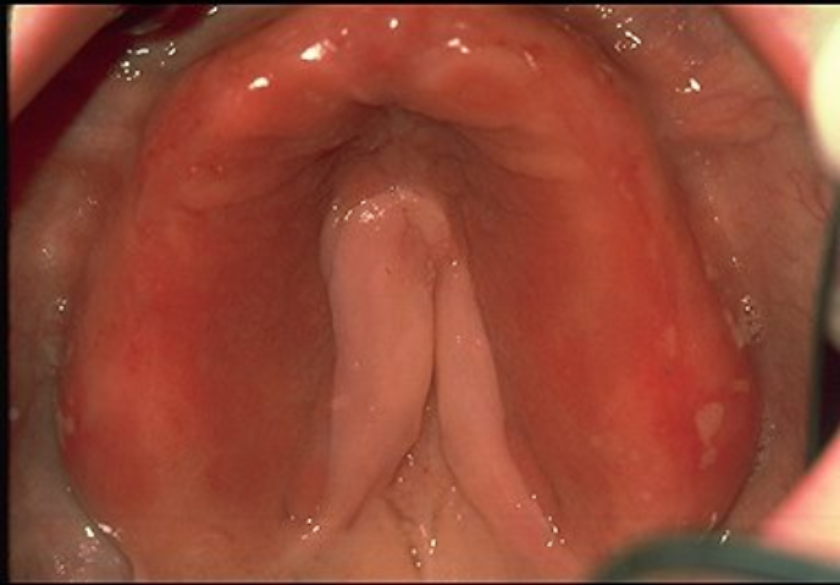
Denture Sore Mouth (Denture-Related Stomatitis)
Denture sore mouth is also known as sore mouth under plates, chronic denture palatitis, stomatitis prosthetica, denture-related candidiasis, denture-induced stomatitis and denture stomatitis.
Nowadays, “denture stomatitis” stands for a mild chronic erythematous candidiasis, usually seen after middle age as erythema (redness) limited to the area beneath an upper denture with the presence of the denture as the only common aetiological factor to these situations. It is not caused by allergy to the denture material.
Epidemiology
Denture stomatitis is a common condition: findings from several studies suggest that it can affect as many as 35 – 50% of persons who wear complete dentures.
The prevalence of denture stomatitis among those wearing partial dentures is markedly lower than among complete denture wearers, whose rank goes from 10 – 70% depending on the population studied.
No racial or sex predilection exists, although some authors have described a higher prevalence among women.
Denture stomatitis lesions may show different clinical patterns and are more frequently found in the upper jaw, especially on the palate (roof of the mouth). The absence of denture stomatitis in the lower jaw is probably due to the washing action of saliva.
Despite the fact that denture stomatitis is frequently asymptomatic, patients may complain of halitosis, slight bleeding and swelling in the involved area or a burning sensation, xerostomia, or taste alterations (dysgeusia). These symptoms occur, with variable intensity, in 20 – 70% of patients with denture stomatitis. In these situations, the patient usually does not relate the use of a denture to the experienced symptoms.
Staging
Different classifications have been proposed, but the reference classification for denture stomatitis is the one suggested by Newton in 1962, based exclusively on clinical criteria:
- Newton´s type I: pin-point hyperæmic lesions (localized simple inflammation)
- Newton´s type II: diffuse erythema confined to the mucosa contacting the denture (generalized simple inflammation)
- Newton´s type III: granular surface (inflamatory papillary hyperplasia)
Predisposing Factors for Oral Candidosis include:
1. Systemic factors
- Physiological (Advanced age)
- Endocrine dysfunctions
- Nutritional deficiencies
- Neoplasias
- Immuno-suppression
- Broad spectrum antibiotics
2. Local factors
- Anti-microbials and topical / inhaled corticosteroids
- Carbohydrate rich diet
- Tobacco and alcohol consumption
- Hypo-salivation
- Deficient oral hygiene
- Wearing dentures (especially through the night)
Treatment
Good oral hygiene is mandatory. The mouth must be kept as clean as possible and a thorough rinse after meals should be performed.
Local factors which promote growth of yeasts, such as smoking or wearing the dentures throughout the night, must be discouraged.
Dentures should be removed for as long as possible and definitely overnight. Dentures should be brushed in warm, soapy water and soaked overnight in an antiseptic solution such as bleach (10 drops of household bleach in a denture cup), chlorhexidine (not when the denture has metal components) or in any solution suitable for sterilizing baby´s feeding bottles. Benzoic acid containing products should be avoided as they induce changes in the composition of acrylic materials.
Denture fitting and occlusal balance should be checked to avoid trauma. A new denture should be made, if necessary. Tissue conditioning agents are porous materials easier to colonize than acrylic, so they are not recommended for these patients. If there is no other choice, an anti-fungal agent, like nystatin, miconazole or ketoconazole may be incorporated to the agent. Dentures must be adequately polished and glazed as pores increase denture contamination by oral micro-organisms
Newton`s type I and II denture stomatitis have been successfully treated with low energy lasers to reduce inflammation of the supporting mucosa. Inflammatory papillary hyperplasia usually needs to be surgically removed (by scalpel, cryosurgery, electro-surgery or with a laser beam) before the denture is placed, although mild cases may respond to anti-fungal treatment.
Anti-fungal medications are recommended when yeasts have been isolated, or when lesions do not resolve with hygiene instructions.
First choice treatment is the topical application of nystatin or miconazole.
Resistance to nystatin is rare; the drug is administered as an oral suspension, with an unpleasant taste and can induce gastro-intestinal problems and hypersensitivity.
Miconazole is available as a gel, varnish, lacquer and chewing gum. It also provokes gastro-intestinal alterations and hypersensitivity, but it tastes better. Miconazole enhances warfarin effect.
Systemic anti-fungal drugs (i.e. fluconazole, itraconazole or ketoconazole) are almost exclusively reserved for patients with systemic factors that condition the development and persistence of candidosis, such as immuno-suppression or diabetes.
Prevention
It is mandatory to include denture stomatitis prevention in oral health care programmes. Dental professionals working with geriatric patients must promote this preventive programmes among all health care workers, home caregivers, members of the patient’s family and, of course, the patients themselves.
A preventive programme should include:
- A routine basis inspection of the oral cavity for screening for this disorder, even when the lesions are asymptomatic.
- Properly denture sanitisation and perform good oral hygiene.
- Appropriate denture-wearing habits, instructing the patient to take their denture out of the mouth for 6 – 8 hours each day.
- Patients with partial dentures should undergo periodic professional plaque control
Useful Articles & Websites
Emedine.com (Denture Stomatitis)
NHS Clinical Knowledge Summaries
British Dental Health Foundation
New Zealand Dermatological Society
Dental Update 2001. Oral Candidosis
Postgrad Med J 2002. Oral Candidiasis
BDJ 2005. Oral Medicine — Update for the dental practitioner. Oral white patches
Aust Dent J 2005. Oral candidosis & the Therapeutic Use of Antifungal Agents in Dentistry
J Appl Oral Sci 2008. Development of Candida-Associated Denture Stomatitis – New Insights
BDJ 2009. Bio-film microbial communities of denture stomatitis
Med Oral Patol Oral Cir Bucal 2011. Candida-Associated Denture Stomatitis
Sheffield Teaching Hospitals NHS Foundation Trust 2014. Denture Related Stomatitis