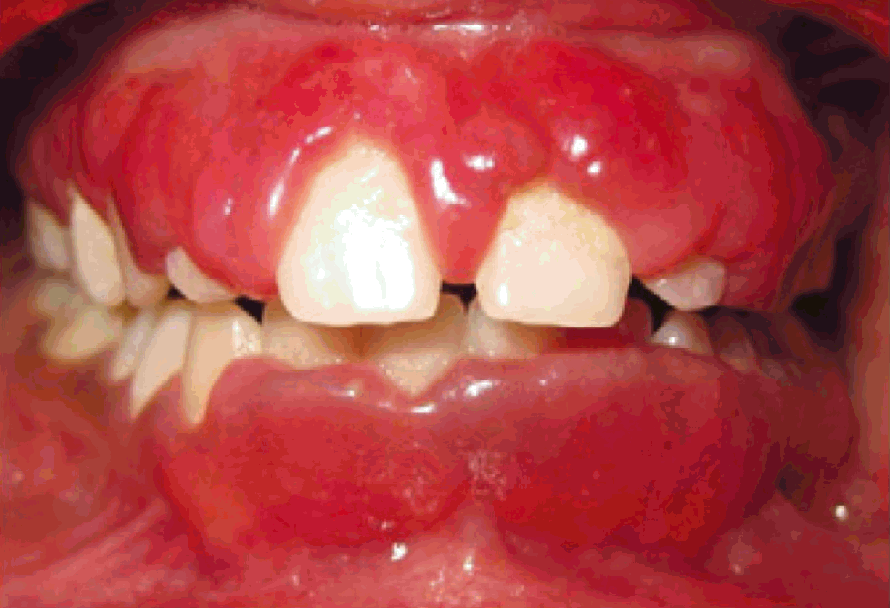
Plasma Cell Gingivitis
Plasma Cell Gingivitis (PCG) is a rare benign condition of the gingiva of unknown ætiology characterised by sharply demarcated erythematous and œdematous gingiva often extending to the muco-gingival junction. PCG is sometimes considered as a hypersensitive reaction.
Plasma Cell Gingivitis is otherwise also known as Atypical Gingivitis, Plasma Cell Gingivostomatitis, Allergic Gingivostomatitis, Soft Tissue Plasmacytosis of the Gingiva, Idiopathic Gingivostomatitis, Stomatitis Venenata or Irritant Contact Stomatitis.
PCG is a rare condition characterized by a massive infiltration of plasma cells into the sub epithelial gingival tissue. Clinically, the illness presents as a diffuse enlargement with œdematous swelling of the gingivæ in the maxillary (upper jaw) and mandibular anterior (lower jaw front) segments. Although the exact mechanism behind this condition is not known, the presence of plasma cells suggests an allergic origin. However, most of the cases seen are without any known or identifiable causes.
What is Plasma Cell Gingivitis?
Plasma Cell Gingivitis (PCG) is a rare benign inflammatory condition of gingivæ (gums) of unknown ætiology characterised by diffuse & massive infiltration of plasma cells into the sub-epithelial gingival tissue.
What are the signs & symptoms of Plasma Cell Gingivitis?
The classical presentation of PCG includes painless, diffuse, erythematous (reddened) and papillary lesions of the gingivæ with a sharp demarcation along the muco-gingival border, which frequently bleeds with minimal trauma. It is more prevalent in young women. Ulceration is rare in the affected gingivæ.
The condition occurs in the anterior gingivæ (ie the gums at the front of the mouth), most frequently in the maxilla (upper jaw).
Plasma cell gingivostomatitis is a similar condition, characterized by a triad of cheilitis (inflammation affecting the lips), glossitis (inflammation affecting the tongue) & gingivitis (inflammation affecting the gums).
What are the causes of Plasma Cell Gingivitis?
This condition has hence been classified into 3 categories, based on the ætiology:
1. PCG due to allergens, such as cinnamon, cinamonaldehyde, chilli, pepper, cardamon or khat leaves.
2. PCG due to neoplastic (cancerous) origin such as multiple myeloma or leukæmia.
3. PCG due to unknown (Idiopathic) cause.
The ætiology is not well defined. It is, most commonly, an immunological / allergic response to the chemicals present in dentifrices (toothpastes), chewing gum, mint pastels and certain foods. It has been suggested that strong spices & some herbs such as chilli, pepper and cardamom may be important factors. The most frequently cited chemical is cinnamon aldehyde (which is widely used as a flavouring agent).
How are they diagnosed?
The diagnosis requires hæmatological & HIV screening in addition to clinical (appearance & a negative Nikolsky sign) & histo-pathological examination (ie a biospy) in order to exclude leukæmia, SLE or Wegener’s Granulomatosis (Granulomatosis with polyangiitis).
How are they treated?
Identification & avoidance of allergen.
Elimination of plaque-retentive factors & maintenance of good oral hygiene.
If these fail or as adjuncts to the above:
- Topical, intra-lesional & systemic corticosteroids
- Tacrolimus
- Antibiotics (Topical application of 2% Fusidic Acid & Chlorpheniramine)
- Antifungals
- Antihistamines (Chlorpheniramine)
- Cryotherapy (Liquid Nitrogen)
- Laser
- Surgical Excision with Gingivectomy
Differential Diagnosis:
- Allergic Contact Mucositis
- Plasmacanthoma
- Solitary Plasmacytoma
- Cheilitis Granulomatosa
- Syphilis
- Candidiasis
- Erythroplasia of Queyrat
- Discoid Lupus
- Oral Lichen Planus
- Cicatricial Pemphigoid
- HIV-Related Gingivitis
- Leukæmia
- Multiple Myeloma
- Waldenströms Macroglobulinæmia
Useful Articles & Websites
BDJ 2002. Plasma Cell Gingivitis apparently related to the Use of Khat. Report of a Case
J Ind Acad Oral Med Radiol 2014. Plasma Cell Gingivitis. A Case Report
BMJ Case Rep 2015. Plasma Cell Gingivitis with Severe Alveolar Bone Loss
J Ind Soc Perio 2015. Plasma Cell Gingivitis
J Clin Diag Res 2016 Plasma Cell Gingivitis – A Conflict of Diagnosis
Oral Maxillofac Pathol J 2017. Gingivitis posing a Diagnostic Dilemma
Int J Curr Adv Res 2019. Plasma Cell Gingivitis – A Case Report & Literature Review
J Dent Oral Sci 2020. Plasma Cell Mucositis – Rare Case Report