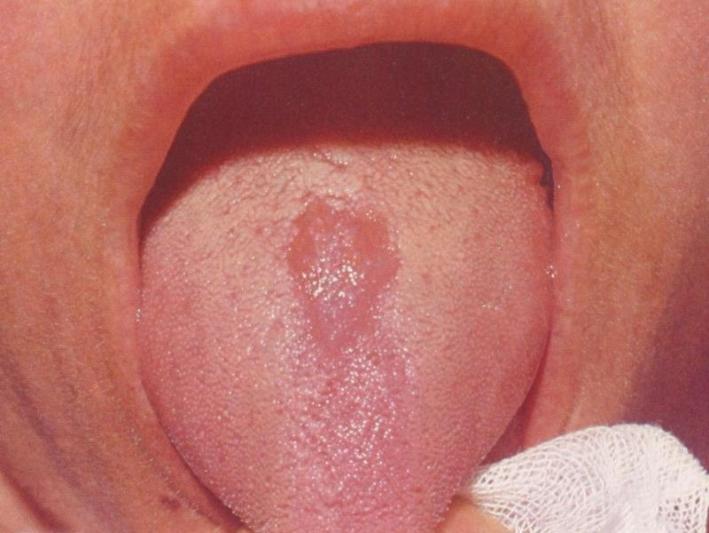
Median Rhomboid Glossitis
Median Rhomboid Glossitis (MRG), also known as Central Papillary Atrophy, Posterior Lingual Papillary Atrophy or Posterior Midline Atrophic Candidiasis, is a type of erythematous candidiasis unique to the midline posterior tongue. It occurs in as many as 1% of adults.
This affects the tongue. There is a central area on the tongue dorsum (just in front of the sulcus terminalis, approx 2/3’s of the way back on the tongue) that has no papillæ (depapillated). This is rhomboid in shape.
What are the causes of Median Rhomboid Glossitis (MRG)?
MRG was once thought to be a developmental defect that occurred during embryogenesis, caused by the failure of the tuberculum impar to be covered completely by the lateral processes of the tongue.
MRG is found anterior to the circumvallate papillæ. Since MRG is not found in children, a developmental ætiology has been largely discounted; however, a direct cause has not been established.
How is it diagnosed?
Prior to biopsy, the clinician should be certain that the midline lesion does not represent a lingual thyroid as it may be the only thyroid tissue present in the patient’s body. Additional clinical look-alike lesions include the gumma of tertiary syphilis, the granuloma of tuberculosis, deep fungal infections and granular cell tumour.
How is it treated?
No treatment is necessary for MRG but nodular cases are often removed for microscopic evaluation.
Anti-fungal therapy (topical troches or systemic medication) will reduce clinical erythema and inflammation due to candida infection. This therapy should ideally be given prior to the biopsy, in order to reduce the candida-induced pseudo-epitheliomatous hyperplasia features.
Some lesions will disappear entirely with anti-fungal therapy.
If the patient is a denture wearer, as with the treatment of any type of candida, the appliances, dentures or any other oral devices should be treated with anti-fungal agents.
Differential diagnosis: Candida infection, chemical burns, syphilis patches depending upon the clinical appearance, geographic tongue, nutritional deficiencies, lichen planus and traumatic ulcerations would be considerations. With any unexplained lesion, oral cancer is always considered, although the centre of the tongue is not a common area for malignancy.
Useful Articles & Websites
Registered Dental Hygienist Magazine
American Association of Oral Medicine
American Academy of Oral Medicine 2007. Patient Information Sheet. Median Rhomboid Glossitis
ENT Journal 2007. Median Rhomboid Glossitis
New Engl J Med 2010. Images in Clinical Medicine. A Smooth Patch on the Tongue
Winter 2010. Pathology Snapshot. Median Rhomboid Glossitis
2014. Median rhomboid glossitis with palatal ‘kissing lesion’. A Case Report
Indian J Case Reports 2018. Atypical Median Rhomboid Glossitis. A Case Report