Oral Aphthous Ulceration
What are recurrent mouth ulcers?
Ulcers are sores that appear inside the mouth and can be itchy or painful. A recurrent ulcer is one that comes and goes, sometimes every few weeks. They are different from cold sores, which appear on the outer lips and are due to a virus infection.
They are common with over 60% of the population suffering from recurrent mouth ulcers at some time in their lives.
Often they begin in childhood, but most people grow out of them by their late twenties. In many cases, several members of the family may suffer from these ulcers, which can be due to a family tendency rather than being passed by infection.
Where do they occur?
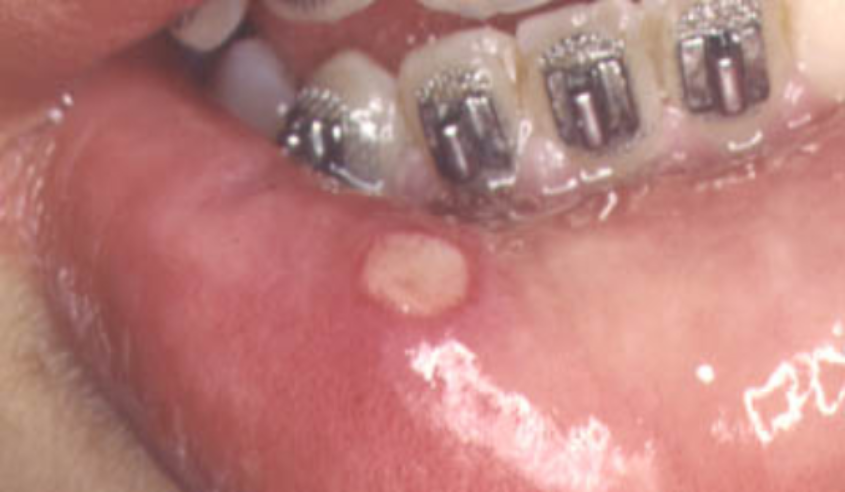
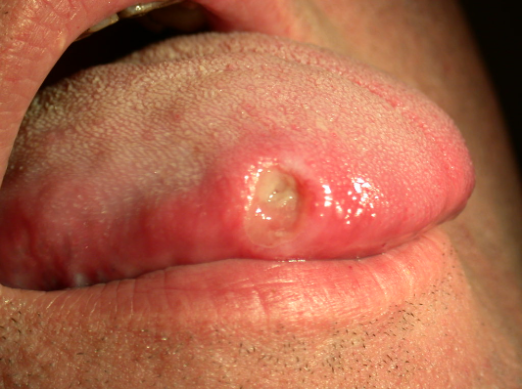
Small ulcers can appear inside the cheeks, on the lips, tongue, gums, and, more rarely, the roof of the mouth.
Most of these ulcers (minor type) are the size of the top of a pencil and can sometimes come in clusters.
Large ulcers (major type) may appear near the tonsils and can be very painful, especially when swallowing.
It is also possible to have up to 100 very small ulcers (herpetiform type). However, these last two types are very rare.
You may get ulcers in other parts of the body, e.g. eyes or genital area. It is important to tell your dentist / doctor about this.
How long do they last for?
The ulcer usually begins with an itchy feeling at the spot where it is due to appear.
After 6 – 24 hours, an ulcer forms and can last 7 – 10 days.
The very large ones can take up to 6 weeks to heal (and often heal by scarring).
What causes mouth ulcers?
Recurrent mouth ulcers cannot be caught by kissing or sharing drinks and utensils, as they are not caused by infection.
They may be an auto-immune disease caused by the body attacking the cells lining the mouth.
It has been suggested that the following factors have a role in causing mouth ulcers:
- Too little dietary iron or a lack of vitamins, especially B12 and C
- Bowel disease, such as Crohn’s disease or ulcerative colitis
- Cœliac disease (gluten sensitivity)
- Hormonal changes; many women get ulcers at the time of their period
- Stress Certain foods
Should I be worried about my mouth ulcers?
No. Most ulcers heal up on their own.
In order to reduce the discomfort, it is important that you keep your mouth clean at all times. Use a diluted chlorhexidine mouthwash once a day. You can buy this at any chemist.
Sprays, rinses and gels are also available for pain relief.
Consult your dentist / doctor if you think you need additional medication or if the ulcers persist.
What can the Clinician do?
You may have a blood test taken and you will probably be prescribed some form of medication to help the ulcer heal faster and so reduce the pain.
However, these medications cannot stop the ulcers from appearing. Most are steroid-based but are safe to use provided they are not swallowed. It is usually recommended to use them as soon as you feel an ulcer starting.
Other medications may be prescribed, if necessary.
How you can treat mouth ulcers yourself
Mouth ulcers need time to heal and there’s no quick fix.
Avoiding things that irritate your mouth ulcer should help:
• speed up the healing process
• reduce pain
• reduce the chance of it returning
Do
• use a soft-bristled toothbrush
• drink cool drinks through a straw
• eat softer foods
• get regular dental check-ups
• eat a healthy, balanced diet
Don’t
• eat very spicy, salty or acidic food
• eat hard, rough, crunchy food, such as toast or crisps or doritos
• drink very hot or acidic drinks, such as fruit juice
• use chewing gum
• use toothpaste containing sodium lauryl sulphate
Pharmacy Medicines:
You can buy several types of mouth ulcer treatment from a pharmacy. Speak to your pharmacist about the best
treatment for you. Options include the following:
• Analgesics (such as paracetamol & ibuprofen)
• Benzocaine lozenges
• Xylocaine 2% gel
• Lidocaine 5% ointment / lozenges or 10% solution spray
• Difflam Mouthwash
• Flurbiprofen lozenges
• Bonjela Dental Gel
• Corsodyl Mouthwash
• Gengigel
• Gelclair
• Orabase
• Combinations: Bonjela Complete Plus & Iglu Rapid Relief Gel
Useful Articles & Websites
Emedicine.com (Ear, Nose & Throat)
British National Formulary (BNF)
NICE Clinical Knowledge Scenarios
BDJ 2005. Nicorandil induced oral ulceration
BDJ 2005. Oral Medicine — Update for the Dental Practitioner. Aphthous and other common ulcers
Oral Biosci Med 2005. Clinical Assessment of Disease Severity in Recurrent Aphthous Stomatitis
BMJ Clinical Evidence 2007. Recurrent Aphthous Ulcers
ENT News 2008. Mouth Ulceration
British Medical Journal 2009. 10-Minute Consultation. Aphthous Ulcers.
Evidence-Based Dentistry 2009. Vitamin B12 for the Treatment of Recurrent Aphthous Stomatitis
BMJ 2010. Evaluation of oral ulceration in primary care
BMJ Best Practice 2014. Mouth Ulcers
BDJ 2014. Content & Quality of Website Information on the Treatment of Oral Ulcers
Dental Update 2015. Clinical Challenges Q&A 11. Ulcers
Dental Update 2015. Clinical Challenges Q&A 13. Painful Lip & Mouth Ulceration
BDJ 2016. Statins & Oral Ulceration
Dental Update 2016. Clinical Challenges Q&A 18. Oral Ulceration
Dental Update 2018. Oral Mucosal Ulceration Induced by Alendronic Acid – A Case Series
British Society of Oral Medicine Information Sheet
Guy’s & St Thomas’ Oral Medicine Clinic. Ulcer Severity Score Sheet